Ngā Kawepūrongo
News
Insights, GP profiles, medical opinion and more.
Categories
Equity

23 September 2022 | Equity
Serious changes needed to achieve transformative change for Pasifika peoples
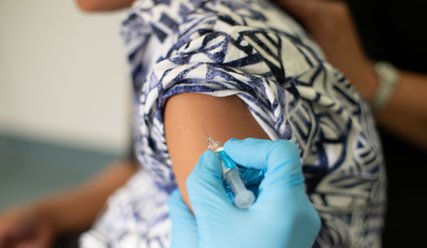
13 September 2022 | Equity
Prioritising Māori and Pasifika for vaccination will save lives

22 August 2022 | Equity
Achieving Equity – working towards better outcomes for Māori patients

5 August 2022 | Equity
Can screening save lives?

3 August 2022 | Equity
Proactive immunisation for Māori tamariki will save lives

1 August 2022 | Equity
Understanding inequity for rural Māori
Upcoming events
See all eventsTURANGA CHRISTCHURCH CENTRAL LIBRARY 60 CATHEDRAL SQUARE CHRISTCHURCH, NEW ZEALAND | CONTINUING MEDICAL EDUCATION
MelNet Skin Lesion and Dermoscopy course
10 May 2024 - 10 May 2024
12:00 PM - 4:30 PM
This beginners’ Skin Lesion and Dermoscopy interactive workshop will describe the typical clinical and dermoscopic characteristics of common benign and malignant skin lesions.
View eventTE PAE CHRISTCHURCH CONVENTION CENTRE 188 OXFORD TERRACE CHRISTCHURCH, 8011 | CONTINUING MEDICAL EDUCATION
Melonoma Mini-Summit
11 May 2024 - 11 May 2024
8:30 AM - 5:00 PM
A critical education opportunity for New Zealand melanoma professionals This one-day Mini-Summit will bring together health professionals working across the continuum of melanoma management.
View eventWebinar: Simplifying HIV prevention
14 May 2024 - 14 May 2024
7:00 PM - 8:00 PM
Simplifying HIV prevention - Updates for prescribing PrEP & PEP.
View eventMore recent articles

6 March 2024 | Clinical
HDC: Botox consent

1 March 2024 | Media releases
GPs working for free to complete crucial patient follow-up – study shows

29 February 2024 | GP Voice
February 2024

28 February 2024 | College and members
Summer Memoir contest results

28 February 2024 | College and members
Summer Memoir contest winner: Dr Lindsay Quennell

28 February 2024 | College and members